HealthArc vs Cadence: User Experience Compared

Choosing the right remote care platform can make or break your practice’s success with chronic care management and remote patient monitoring. HealthArc vs Cadence comparison reveals two very different approaches to healthcare platform user experience – one built for small practices seeking comprehensive support, the other designed for large health systems with protocol-driven care models.
This comparison is for small to mid-sized practices, solo practitioners, and healthcare administrators evaluating remote care solutions. You need to understand which platform actually fits your team size, technical resources, and patient population before committing to a long-term partnership.
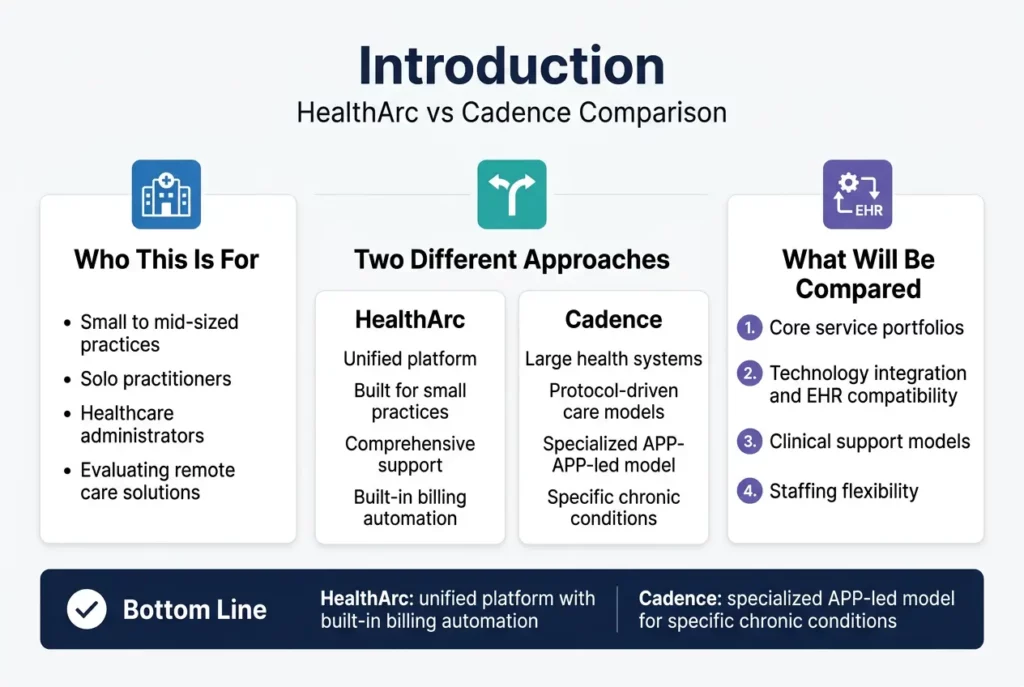
We’ll break down their core service portfolios to show you exactly what each platform offers beyond basic RPM. You’ll also discover how their technology integration and EHR compatibility differs – especially important if you’re working with limited IT support. Finally, we’ll compare their clinical support models and staffing flexibility so you can see which approach matches your practice’s capacity and care philosophy.
By the end, you’ll know whether you need HealthArc’s unified platform with built-in billing automation or Cadence’s specialized APP-led model for specific chronic conditions.
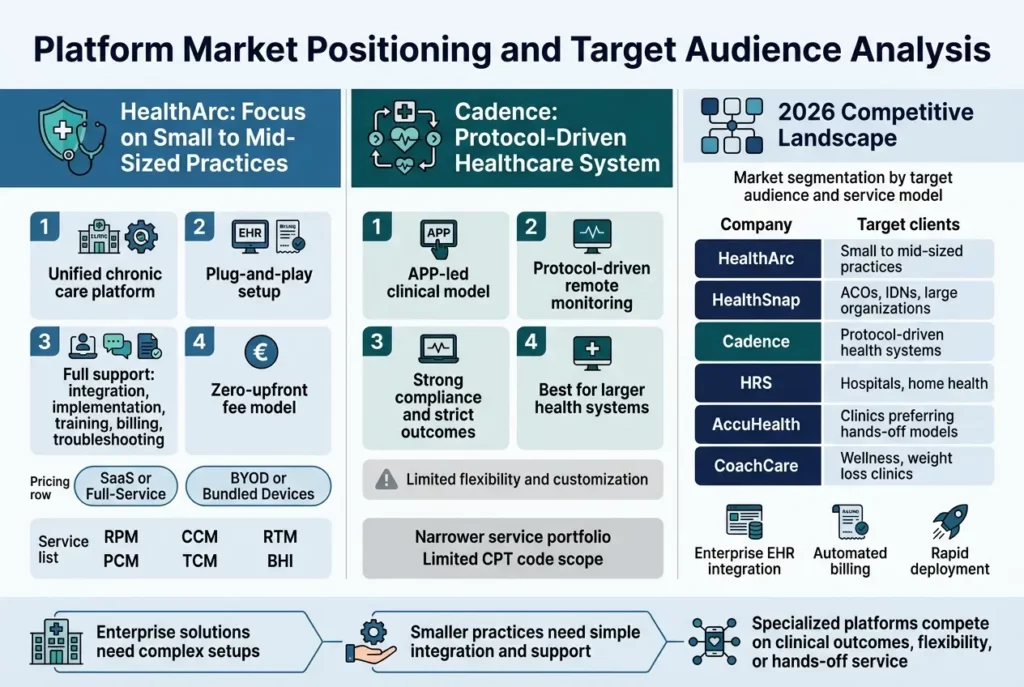
HealthArc’s Focus on Small to Mid-Sized Practices
HealthArc strategically positions itself as a unified chronic care management platform designed specifically for small to mid-sized practices. Unlike enterprise-focused solutions that demand extensive resources and complex implementations, HealthArc offers a plug-and-play system that supports scalability without overwhelming smaller care teams. This healthcare platform user experience is built around the understanding that small practices often lack in-house tech support or billing teams.
The platform addresses critical pain points for smaller providers by offering comprehensive support across integration, implementation, training, billing, and troubleshooting. This makes remote care integration seamless for practices that cannot afford the resource-intensive setups required by larger competitors. HealthArc’s value-based outcomes approach ensures that small practices can successfully scale their remote services without significant capital investment, featuring a zero-upfront fee model that reduces barriers to entry.
Key differentiators for small practices include flexible pricing options based on SaaS or full-service preferences, the ability to choose between bundled device models or bring-your-own-device (BYOD) setups, and transparent, scalable pricing structures. The platform’s medical practice management software capabilities extend across Remote Patient Monitoring (RPM), Chronic Care Management (CCM), Remote Therapeutic Monitoring (RTM), Principal Care Management (PCM), Transitional Care Management (TCM), and Behavioral Health Integration (BHI).
Cadence’s Protocol-Driven Healthcare System Approach
Cadence operates with a distinctly different market positioning, focusing on APP-led clinical models with a protocol-driven approach to remote monitoring. This healthcare technology implementation strategy targets larger healthcare systems that can support specialized clinical roles and medical infrastructure, which smaller clinics often lack. Cadence’s service model demonstrates impressive clinical outcomes, including a recently promoted 50% reduction in hypertension patients, but these results are typically achieved through large-scale pilot programs and hospital collaborations.
The platform’s strength lies in its disease-specific, protocol-driven approach that offers strict compliance and strong protocol-based outcomes. However, this focus comes with limited flexibility and customization options, making it less suitable for practices requiring adaptable care plans. Cadence’s APP-led care team model effectively reduces patient escalations but demands substantial infrastructure investment that may not align with smaller practice capabilities.
Notably, Cadence’s service portfolio is narrower compared to comprehensive platforms, lacking distinct Chronic Care Management services and offering limited CPT code scope for billing optimization. This clinical support models approach works well for protocol-driven health systems but may not provide the billing flexibility that diverse practices require for revenue optimization.
Competitive Landscape Overview for 2026
The competitive landscape for healthcare platform user experience in 2026 reveals distinct market segmentations based on target audiences and service delivery models. The market divides into several key categories: unified chronic care platforms targeting small to mid-sized practices, enterprise virtual care solutions for large organizations, protocol-driven systems for specialized healthcare environments, and turnkey monitoring services for hands-off providers.
| Company | Market Focus | Target Clients |
|---|---|---|
| HealthArc | Unified chronic care | Small to mid-sized practices |
| HealthSnap | Enterprise virtual care | ACOs, IDNs, large organizations |
| Cadence | APP-led RPM | Protocol-driven health systems |
| HRS | Telehealth + RPM | Hospitals, home health |
| AccuHealth | Turnkey 24/7 monitoring | Clinics preferring hands-off models |
| CoachCare | Virtual health suite | Wellness, weight loss clinics |
This landscape demonstrates how EHR integration comparison and medical billing automation capabilities vary significantly based on target market focus. Enterprise solutions like HealthSnap offer compatibility with 80+ EHR systems but require complex setups and extensive resources. Meanwhile, platforms targeting smaller practices prioritize simplified integration and automated billing processes.
The competitive environment shows increasing specialization, with each platform developing distinct strengths: some focus on comprehensive service portfolios, others on rapid deployment, and still others on specific clinical outcomes. This specialization creates opportunities for practices to select platforms that align with their operational capacity, technical requirements, and patient care objectives, making the selection process more strategic than ever before.
Core Service Portfolio Comparison
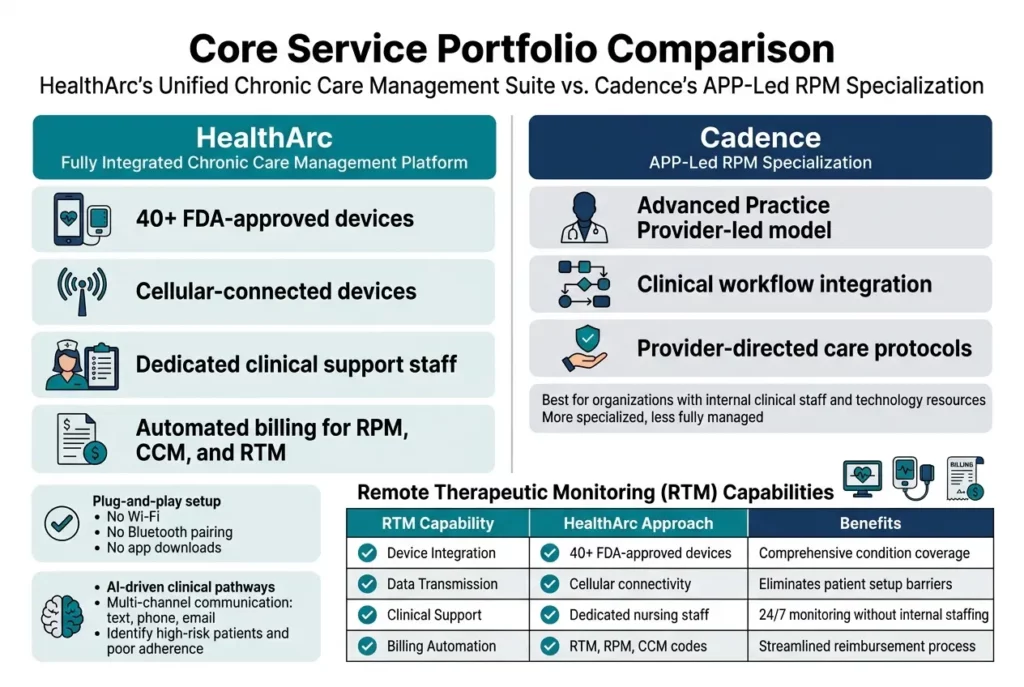
HealthArc’s Unified Chronic Care Management Suite
HealthArc delivers a comprehensive, fully integrated chronic care management platform that distinguishes itself through its end-to-end service model. Unlike software-only solutions, HealthArc provides a complete package that includes cellular-connected medical devices, dedicated clinical support staff, and automated billing systems, all designed to streamline remote patient monitoring operations.
The platform supports over 40 FDA-approved health devices, including blood pressure cuffs, glucose monitors, pulse oximeters, and ECG monitors from trusted brands like Roche and Dexcom. A key advantage lies in the cellular connectivity of these devices, which eliminates the complexity of Wi-Fi setup, Bluetooth pairing, or app downloads for patients. This plug-and-play approach significantly improves patient adherence and reduces technical barriers that often hinder remote monitoring success.
HealthArc’s AI-driven clinical pathways can be customized to specific practice needs, enabling clinicians to quickly identify high-risk patients or those showing poor adherence to treatment protocols. The platform facilitates multi-channel communication through text, phone, or email based on patient preferences, ensuring optimal engagement strategies.
Perhaps most significantly, HealthArc includes a dedicated pod of clinical support staff comprising enrollment specialists, nurses, and medical assistants who handle patient onboarding, follow-up calls, and daily monitoring. This embedded workforce extends the practice’s clinical footprint without requiring additional internal hiring, making it particularly valuable for organizations with limited staffing resources.
Cadence’s APP-Led RPM Specialization
Based on the reference content, Cadence appears to focus on Advanced Practice Provider (APP)-led RPM specialization, though specific details about Cadence’s service portfolio are not extensively covered in the provided materials. The healthcare platform user experience comparison suggests that Cadence positions itself as a more specialized solution compared to HealthArc’s comprehensive approach.
The APP-led model typically emphasizes clinical workflow integration and provider-directed care protocols, allowing healthcare organizations to maintain direct clinical oversight while leveraging technology for remote monitoring capabilities. This approach appeals to practices that prefer to retain primary clinical responsibility while utilizing technology platforms to extend their reach and monitoring capabilities.
Organizations considering this model should evaluate their existing clinical staff capacity and technology infrastructure, as APP-led solutions often require more internal resource allocation compared to fully managed platforms like HealthArc.
Remote Therapeutic Monitoring Capabilities
Remote Therapeutic Monitoring (RTM) represents an advanced capability that extends beyond traditional vital sign monitoring to include therapeutic interventions and treatment adherence tracking. HealthArc’s platform demonstrates robust RTM capabilities through its comprehensive device ecosystem and automated billing support for RTM codes.
The platform’s RTM functionality encompasses monitoring of respiratory therapy devices, pain management tools, and medication adherence systems. HealthArc’s automated billing system handles documentation and claims submission for RTM services alongside RPM and Chronic Care Management (CCM) codes, reducing administrative burden and ensuring proper reimbursement optimization.
| RTM Capability | HealthArc Approach | Benefits |
|---|---|---|
| Device Integration | 40+ FDA-approved devices | Comprehensive condition coverage |
| Data Transmission | Cellular connectivity | Eliminates patient setup barriers |
| Clinical Support | Dedicated nursing staff | 24/7 monitoring without internal staffing |
| Billing Automation | RTM, RPM, CCM codes | Streamlined reimbursement process |
The cellular-enabled devices ensure consistent data flow without requiring patient technical expertise, while the dedicated clinical team provides the specialized monitoring required for effective RTM programs. This combination addresses the dual challenges of patient engagement and clinical oversight that often limit the success of remote therapeutic monitoring initiatives.
HealthArc’s RTM capabilities are particularly valuable for managing complex chronic conditions requiring ongoing therapeutic intervention monitoring, such as diabetes management with continuous glucose monitoring or cardiac care with remote ECG surveillance.
Technology Integration and EHR Compatibility
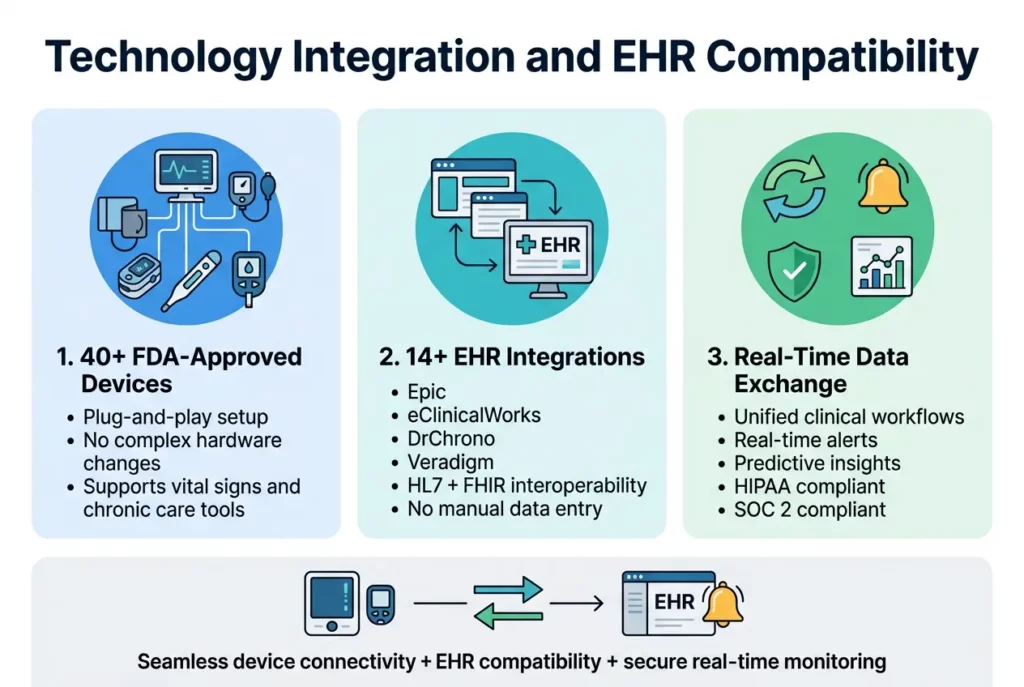
HealthArc’s Plug-and-Play FDA-Approved Devices
HealthArc’s platform demonstrates superior device connectivity through its seamless integration with 40+ medical devices. This extensive compatibility ensures healthcare providers can leverage their existing equipment while implementing remote patient monitoring solutions without significant hardware investments. The platform’s plug-and-play architecture eliminates complex setup procedures, allowing clinical teams to quickly deploy monitoring capabilities across various patient populations.
The broad device compatibility spans multiple categories of FDA-approved medical equipment, from basic vital sign monitors to specialized chronic disease management tools. This flexibility enables healthcare organizations to customize their remote monitoring programs based on specific patient needs and clinical protocols without being constrained by device limitations.
Deep HL7 and FHIR Integration Benefits
Now that we’ve explored device compatibility, HealthArc’s EHR integration comparison reveals significant advantages in interoperability standards. The platform seamlessly integrates with 14+ EHR systems, including industry leaders such as Epic, eClinicalWorks, DrChrono, and Veradigm. This comprehensive EHR compatibility ensures that healthcare organizations can maintain their existing electronic health record workflows while adding advanced remote care capabilities.
The integration eliminates manual data entry requirements, significantly reducing administrative burden on clinical staff. Healthcare providers can access patient records directly within the HealthArc portal, creating a unified workspace that enhances clinical efficiency. This streamlined approach to healthcare technology implementation reduces the risk of data entry errors while improving overall workflow productivity.
Seamless Data Exchange and Real-Time Alerts
Previously established EHR connections enable sophisticated data exchange capabilities that transform clinical decision-making processes. HealthArc’s platform provides unified communication and streamlined clinical workflows through real-time data synchronization between remote monitoring devices and existing health records systems.
The platform’s analytics module generates real-time data insights that enable healthcare providers to identify health patterns, trends, and provide predictive insights for improved patient outcomes. This continuous data flow supports proactive care management by alerting clinical teams to potential health concerns before they escalate into serious complications.
With HIPAA and SOC 2 compliance standards maintained throughout all data exchanges, the platform ensures the highest levels of data security and patient privacy while facilitating seamless information flow between systems.
Clinical Support Models and Staffing Flexibility
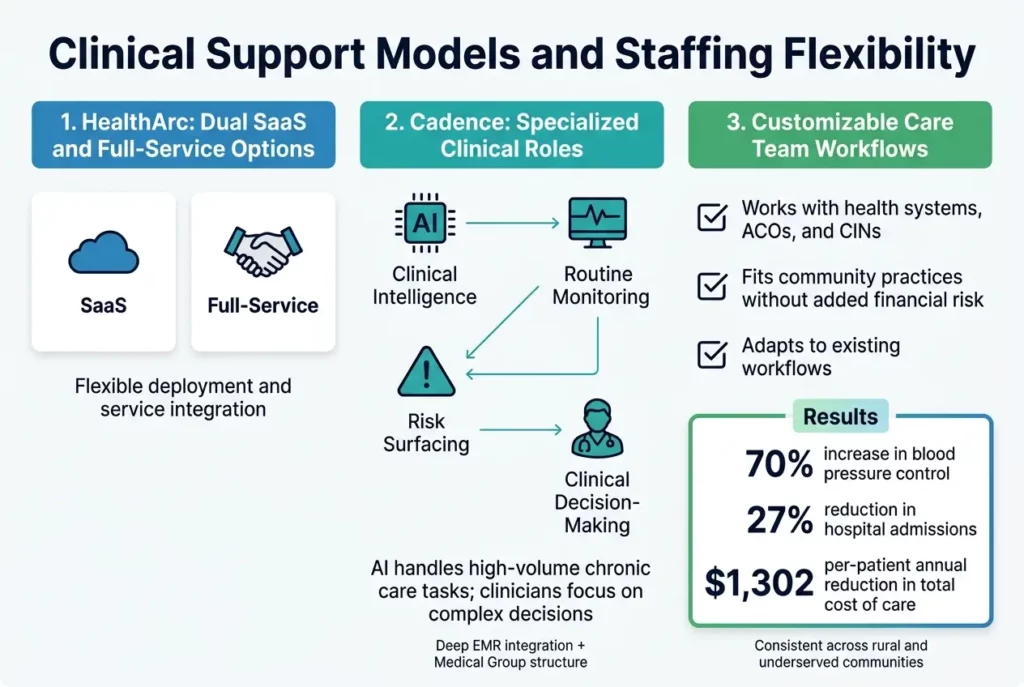
HealthArc’s Dual SaaS and Full-Service Options
Based on the available information, the clinical support models in the healthcare platform comparison reveal distinct approaches to delivering care. While specific details about HealthArc’s dual SaaS and full-service offerings are not extensively documented in the reference materials, the healthcare technology landscape demonstrates varying levels of service integration and deployment flexibility that healthcare organizations require when selecting platforms.
Cadence’s Specialized Clinical Role Requirements
Cadence has established itself as the nation’s leading remote patient care system with a comprehensive clinical support framework that emphasizes specialized role requirements. The platform operates through an AI-native program that builds on a demonstrated track record of driving measurable outcomes across entire populations. Since 2021, Cadence has partnered with more than 20 leading health systems to co-develop and deploy technology-enabled care models, successfully serving over 130,000 patients while strengthening local physician relationships.
The clinical support model at Cadence centers around its Clinical Intelligence system, which takes on the routine, high-volume work of chronic care including monitoring patients, surfacing risks, and coordinating action. This approach allows clinicians to focus specifically on decisions that require their expertise, creating a specialized role structure where AI handles data processing and routine monitoring while healthcare professionals concentrate on complex clinical decision-making.
Cadence’s staffing model is grounded in partnerships with leading health systems, deep EMR integration capabilities, and its own Medical Group structure. This integrated approach ensures that clinical staff can work within established workflows while leveraging advanced technology to enhance patient care delivery.
Customizable Care Team Workflows
Now that we’ve examined the clinical support structures, it’s important to understand how these platforms enable customizable care team workflows. Cadence’s system demonstrates significant flexibility in workflow customization through its partnership-based approach with health systems, Accountable Care Organizations, and Clinically Integrated Networks.
The platform’s workflow customization extends directly into community practices without adding financial risk or administrative burden for physicians. This model allows care teams to maintain their existing processes while integrating advanced chronic disease management capabilities. The system’s AI-powered remote care model can be adapted to work with affiliated physicians across different practice settings, demonstrating the platform’s ability to accommodate varying workflow requirements.
Clinical outcomes data from Cadence programs show the effectiveness of these customizable workflows, with patients achieving a 70% increase in blood pressure control, a 27% reduction in hospital admissions, and a $1,302 per-patient annual reduction in total cost of care. These results remain consistent across rural and underserved communities, indicating that the workflow customization capabilities can be successfully implemented across diverse healthcare settings and patient populations.
The Clinical Intelligence system’s ability to surface risks and coordinate action provides care teams with the flexibility to customize their response protocols while maintaining consistent monitoring and intervention capabilities across their patient populations.
Billing Automation and Reimbursement Optimization
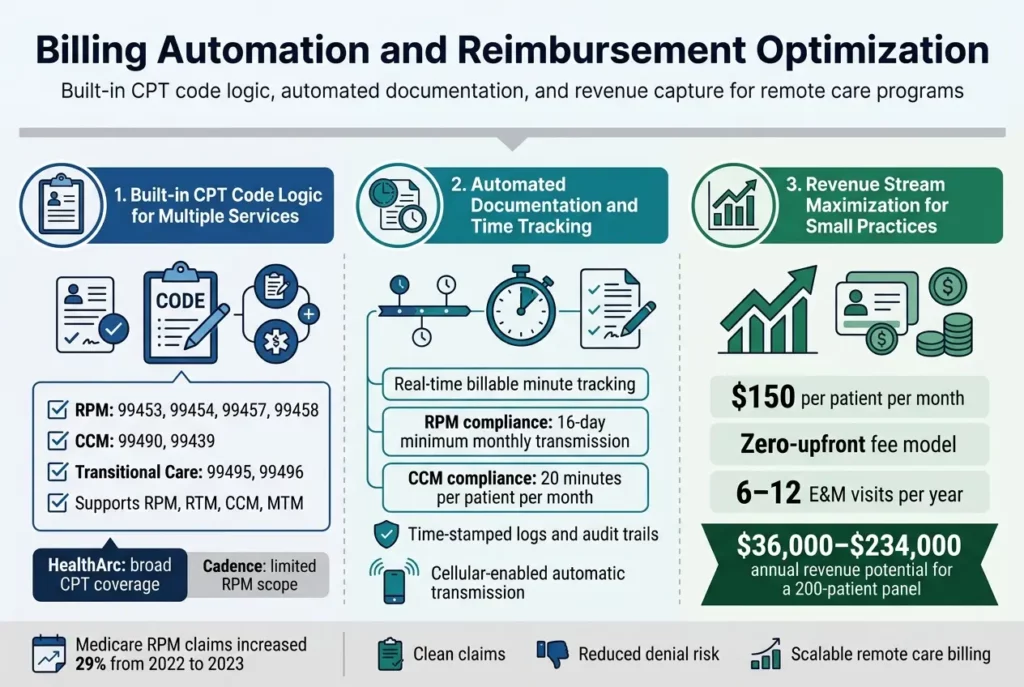
Built-in CPT Code Logic for Multiple Services
HealthArc stands out in the healthcare platform landscape by offering comprehensive built-in CPT code logic that spans multiple remote monitoring and care management services. The platform provides automated billing support for RPM, RTM, CCM, MTM, and other remote monitoring services, eliminating the complexity that small practices typically face when navigating complex reimbursement codes.
Unlike Cadence, which operates with limited CPT scope focusing primarily on protocol-driven RPM services, HealthArc’s platform includes extensive coverage across diverse service lines. The built-in logic ensures that providers can confidently handle various billing scenarios without requiring specialized billing staff or external consultants. This comprehensive approach to billing automation represents a significant advantage for small and mid-sized practices that lack dedicated back-office coding teams.
The platform’s CPT code coverage includes support for Medicare reimbursement across multiple service categories. For RPM services, this encompasses device supply and data collection (99454), clinical time billing (99457, 99458), and setup codes (99453). Additionally, HealthArc supports CCM billing codes (99490, 99439) and transitional care management codes (99495, 99496), providing practices with the ability to capture revenue from multiple care coordination activities under one integrated system.
Automated Documentation and Time Tracking
HealthArc’s platform addresses one of the most critical challenges in medical billing automation: accurate documentation and time tracking for compliance purposes. The system automatically tracks billable minutes in real time, ensuring that practices meet the specific compliance thresholds required for successful reimbursement claims.
For RPM billing compliance, the platform monitors device transmission patterns to ensure patients meet the 16-day minimum threshold required for monthly billing. This automated tracking eliminates manual oversight burdens and reduces the risk of unbillable months due to missed compliance requirements. The system’s cellular-enabled devices support automatic data transmission, which significantly improves patient compliance rates compared to Bluetooth-dependent solutions that rely on manual patient action.
The documentation automation extends to CCM services, where the platform tracks and documents the required 20 minutes of care coordination activities per patient per month. This automated approach ensures clean claim submission and reduces the administrative burden on care coordinators who would otherwise need to manually track and document these activities across large patient panels.
HealthArc’s time-stamped logs and audit trails provide the detailed records necessary for CMS compliance and payer scrutiny. As RPM claims volumes continue to grow, with Medicare data showing a 29% increase from 2022 to 2023, automated documentation becomes increasingly valuable for maintaining clean billing practices and avoiding claim denials.
Revenue Stream Maximization for Small Practices
The platform’s integrated approach to billing automation directly translates to revenue stream maximization for small practices. By combining automated documentation, compliance tracking, and comprehensive CPT code support, HealthArc enables practices to capture revenue opportunities that might otherwise be missed in manual or fragmented billing systems.
For a typical small practice managing chronic patients through both RPM and CCM services, the revenue potential per patient can reach approximately $150 per month in Medicare reimbursement. This includes baseline RPM and CCM codes, with additional opportunities for extended care coordination time and transitional care management services. The platform’s automated systems ensure that practices can consistently capture these revenue opportunities without the staffing overhead typically required for manual billing management.
The zero-upfront fee model further enhances revenue maximization by eliminating capital investment barriers that prevent small practices from launching comprehensive remote care programs. This pricing structure, combined with transparent, scalable fees, allows practices to grow their programs incrementally while maintaining predictable cost structures.
HealthArc’s billing automation capabilities become particularly valuable when considering the downstream revenue effects of improved patient engagement. Enrolled patients typically generate 6-12 evaluation and management visits per year compared to 2-3 for unmanaged chronic patients, creating additional revenue streams worth $36,000-$234,000 annually for a 200-patient panel.
Patient Engagement and Communication Features
Multi-Channel Support System Integration
HealthArc delivers comprehensive patient engagement through intelligent multi-channel communication strategies that leverage SMS, email, phone calls, and in-office collateral materials. The platform’s AI-driven communication system automatically escalates patient interactions based on engagement levels and clinical needs, ensuring no patient falls through the cracks. This omni-channel solution integrates seamlessly with existing EHR systems, enabling healthcare providers to maintain consistent communication workflows across all touchpoints.
The platform’s unified care system employs pod-based teams of enrollment specialists, RNs, LPNs, and medical assistants who coordinate patient outreach campaigns. These intelligent campaigns promote adoption through multiple touchpoints, allowing healthcare teams to scale flexibly without internal overhead or workflow disruption. The automation capabilities enable clinical teams to focus strategically on high-risk or non-compliant patients who require immediate intervention.
Device Setup and User Experience Design
HealthArc’s Device-as-a-Service (DaaS) model provides cellular-enabled medical devices that offer plug-and-play functionality for effortless patient activation. The platform supports over 40 medical devices across various disease types, unifying data from cellular, Bluetooth, and wearable devices from leading brands including Roche, Abbott, Dexcom, Nonin, A&D, and Apple. This singular device portal eliminates the complexity typically associated with multi-vendor device management.
The cellular-enabled IoT medical devices operate independently without requiring Wi-Fi connections or monthly plans, automatically transmitting patient data in real-time. HealthArc manages comprehensive device lifecycle support including ordering, shipping, onboarding, and inventory management through dedicated device management software. The platform incorporates next-generation gamification techniques to enhance patient training and adherence, creating an intuitive experience that encourages consistent device usage and data collection.
Compliance and Satisfaction Improvement Strategies
HealthArc’s AI-powered clinical pathways are configurable for each disease type based on provider feedback, ensuring compliance with clinical protocols while maintaining flexibility for practice-specific requirements. The platform’s predictive analytics capabilities enable proactive interventions that can include recommending doctor visits, specialist referrals, or providing coaching for patient self-management. This Care-as-a-Service (CaaS) approach allows care coordinators to continually review patient vitals through the provider dashboard for timely decision support.
The platform enhances patient satisfaction through personalized health monitoring that reduces the need for in-person visits while maintaining high-quality care standards. Real-time data transmission combined with AI-assisted coaching keeps patients engaged with their treatment plans and health goals. HealthArc provides comprehensive support including 24-hour phone, online chat, and email assistance, ensuring patients receive immediate help when needed. The platform’s billing documentation automation across RPM, CCM, PCM, RTM, and TCM codes streamlines compliance requirements while optimizing reimbursement processes for healthcare providers.
Implementation and Deployment Process
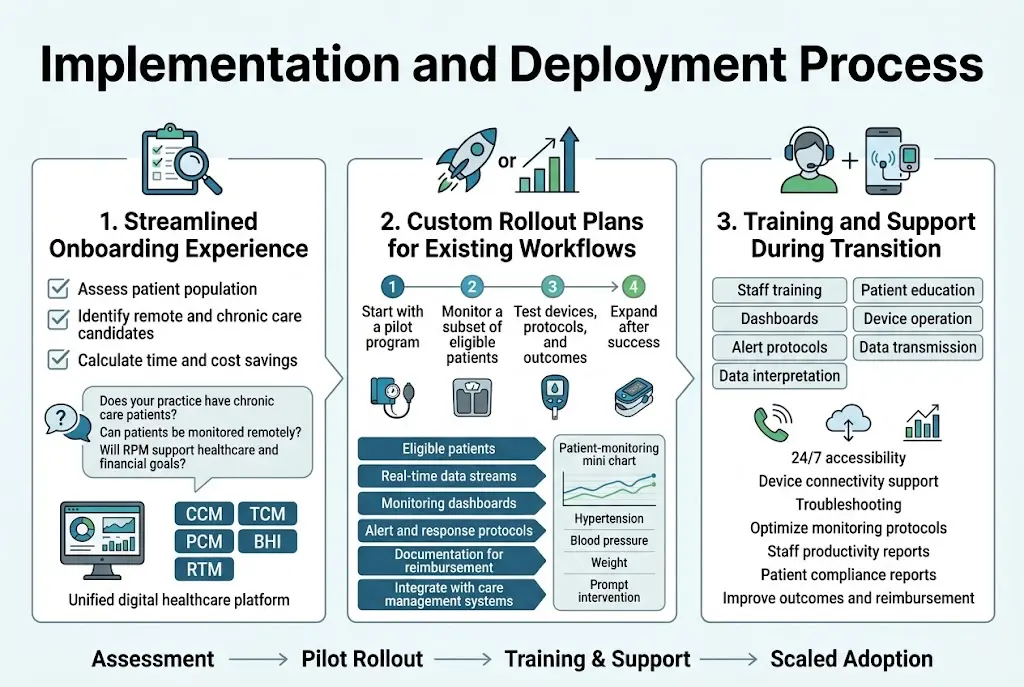
Streamlined Onboarding Experience
HealthArc prioritizes a patient-centered approach to remote patient monitoring implementation that begins with comprehensive assessment and planning. The platform’s onboarding process starts by evaluating key factors that determine implementation success, including analyzing how many patients could benefit from remote monitoring, identifying patients who reside remotely, and calculating potential time and cost savings for both patients and providers.
The streamlined onboarding experience focuses on answering critical questions before technology deployment: Does your practice have a significant number of chronic care patients? Do patients require frequent visits but could be monitored remotely? Will the RPM program help achieve healthcare and financial goals? This methodical assessment ensures that healthcare technology implementation aligns with practice objectives from day one.
HealthArc’s unified digital healthcare platform accommodates multiple monitoring services including Chronic Care Management (CCM), Transitional Care Management (TCM), Principal Care Management (PCM), Behavioral Health Integration (BHI), and Remote Therapeutic Monitoring (RTM) within a single dashboard. This comprehensive approach simplifies the learning curve for both patients and physicians, resulting in better technology adoption and utilization rates.
Custom Rollout Plans for Existing Workflows
Now that we have covered the foundational assessment phase, the implementation process moves into customized deployment strategies. HealthArc recommends starting with a pilot program approach to minimize workflow disruption while maximizing learning opportunities. Healthcare providers can begin with a subset of eligible patients to test device deployment, monitoring protocols, and clinical outcomes before scaling the program.
For example, a physician or care coordinator can initially track vital signs such as blood pressure and weight for patients suffering from hypertension. When significant changes occur in health readings, providers can intervene promptly and make relevant adjustments to care plans. Once satisfied with the workflow and clinical outcomes, practices can expand the RPM program to cover additional patients and conditions.
The custom rollout process requires specific workflow adjustments including: identifying eligible patients based on chronic conditions, deploying FDA-approved remote patient monitoring devices such as pulse oximeters, weighing scales, and glucometers, setting up real-time data streams, establishing monitoring dashboards, defining alert and response protocols, ensuring proper documentation for reimbursement purposes, and integrating RPM data into existing care management systems.
Training and Support During Transition
With this implementation foundation in mind, HealthArc provides comprehensive training and support to ensure successful technology adoption. The platform emphasizes education and clear communication as essential components for maintaining patient engagement throughout the transition period. Patients must understand the purpose of remote monitoring, learn how to properly use connected devices, and recognize the value of consistent data reporting.
The training process covers both technical and clinical aspects of the remote patient monitoring platform. Healthcare staff receive guidance on monitoring dashboards, alert protocols, and data interpretation, while patients learn device operation and data transmission procedures. HealthArc’s cellular medical devices connect seamlessly with the software platform, allowing patients to record and transmit health readings from any location at any time.
Support during transition includes ongoing assistance with device connectivity issues, troubleshooting technical problems, and optimizing monitoring protocols based on early implementation feedback. The platform’s 24/7 accessibility ensures that both patients and providers can access support when needed, reducing implementation barriers and improving adoption rates.
Healthcare providers benefit from staff productivity reports and patient compliance reports that help identify areas for improvement during the transition phase. These analytics enable practices to refine their remote patient monitoring workflows and ensure the program delivers both clinical value through improved patient outcomes and financial returns through enhanced reimbursement opportunities.
Pricing Transparency and Cost Structure
Zero-Upfront Fee Model Benefits
HealthArc’s pricing model eliminates the significant upfront device procurement costs that plague traditional RPM implementations. With their device-as-a-service (DaaS) model, practices receive cellular-enabled medical devices at no initial cost, removing the typical $50-$150 per device expense that competitors require separately. This approach transforms device management from a capital expenditure into an operational one, improving cash flow for growing practices.
The cellular device advantage extends beyond cost savings to revenue protection. Industry data shows patient compliance rates average around 55% with Bluetooth-dependent devices, while cellular auto-transmit devices achieve 80-90% compliance. For a 200-patient panel, this compliance gap translates to approximately $108,000 in lost annual revenue. HealthArc’s zero-upfront model includes these higher-performing cellular devices, ensuring practices capture maximum reimbursement potential from the start.
Flexible SaaS vs Full-Service Pricing Options
When evaluating healthcare platform pricing, practices must look beyond the per-patient monthly fee to understand total cost of ownership. Point solutions that appear cheaper at $15-$20 per patient often require additional investments in device logistics, billing automation, EHR integration, and patient support services. These hidden costs frequently exceed the transparent pricing of integrated platforms.
HealthArc’s all-inclusive pricing model incorporates device management, automated billing workflows, FHIR/HL7 EHR integration, and HIPAA-compliant infrastructure. A comparative analysis shows that a 100-patient RPM program using point solutions generates approximately $99,000 annually due to compliance failures, while HealthArc’s integrated approach delivers $144,000-$162,000 through superior billing automation and patient engagement features.
Scalable Investment for Growing Practices
The architectural differences between platforms become more pronounced as practices scale their remote patient monitoring programs. HealthArc’s AI-powered risk scoring and automated workflows enable care coordinators to manage larger patient panels effectively. A practice with 200 RPM patients typically requires 1-1.5 FTEs with manual workflows, but can operate with 0.5-1 FTE using HealthArc’s automated tools, reducing labor costs by $25,000-$50,000 annually.
Healthcare reimbursement optimization becomes critical at scale. Medicare reimbursement for patients enrolled in both RPM and CCM can reach $150 per month per patient, representing $360,000 annually for a 200-patient panel. HealthArc’s automated billing compliance and denial prevention features ensure practices capture this revenue consistently, while medical billing automation reduces administrative overhead as programs expand.
The compounding effect of higher engagement rates generates additional downstream revenue through increased evaluation and management visits. Patients in active RPM programs schedule 6-12 annual visits compared to 2-3 for unmanaged patients, creating $36,000-$234,000 in incremental revenue for a 200-patient panel.
Conclusion
For small and mid-sized practices evaluating remote care platforms, the choice between HealthArc and Cadence reveals distinct approaches to healthcare delivery. While Cadence excels in protocol-driven, app-led care with impressive clinical outcomes for specific conditions, HealthArc offers a comprehensive, unified platform designed specifically for smaller practices lacking extensive IT infrastructure. The comparison across market positioning, core services, technology integration, clinical support, billing automation, patient engagement, implementation processes, and pricing transparency demonstrates that HealthArc provides the flexibility and simplicity that smaller providers need to succeed in value-based care.
HealthArc’s zero-upfront fee model, built-in CPT code logic, FDA-approved cellular devices, and dual SaaS/full-service options create an accessible pathway for practices to expand their care capabilities without enterprise-level complexity. The platform’s comprehensive service portfolio covering RPM, CCM, RTM, PCM, TCM, and BHI under one dashboard, combined with transparent pricing and streamlined onboarding, positions it as the optimal choice for providers seeking immediate operational improvements and sustainable revenue growth. Ready to transform your practice with unified chronic care management? Schedule a consultation with HealthArc’s expert team to discover how our platform can enhance your patient outcomes while simplifying your remote care operations.
Most Recent Blogs
Categories
Related Blog
- May 8, 2026 | Read Time: 11 mins
How Remote Patient Monitoring is Transforming Primary Care in 2026
As of 2026, primary care does not only exist within the walls...
Learn More- April 28, 2026 | Read Time: 12 mins
Why HealthArc’s Higher Price Tag Pays for Itself: A Real ROI Breakdown
When a practice manager sits down to compare RPM and CCM platforms,...
Learn More- | Read Time: 12 mins
CMS Reporting Requirements: What Providers Must Know
The United States has one of the most highly regulated healthcare sectors...
Learn More